Why Choosing the Right Mental Health Billing Services Company in USA Can Transform Your Practice Revenue
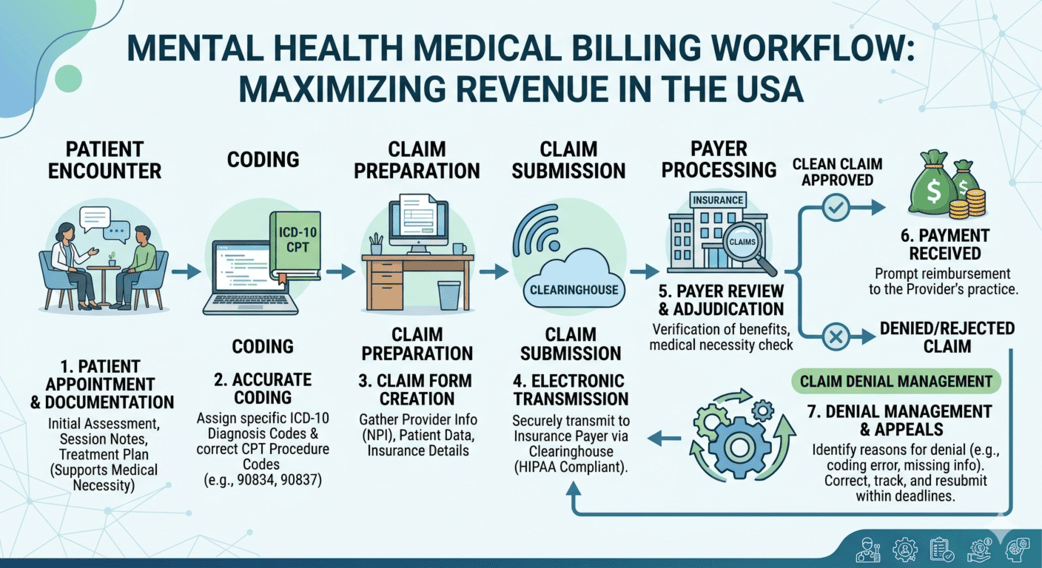
Mental health practices across the USA are growing rapidly—but so are the administrative challenges that come with them. From complex payer rules to evolving compliance requirements, billing for mental health providers has become far more than just submitting claims. It’s a strategic function that directly impacts revenue, patient satisfaction, and operational efficiency.
For therapists, psychiatrists, and behavioral health clinics, partnering with a reliable mental health billing services company is no longer optional—it’s a necessity. This article explores how modern mental health billing solutions can streamline operations, reduce denials, and help practices thrive financially.
The Growing Complexity of Mental Health Billing in the USA
Unlike general medical billing, billing for mental health services involves unique challenges:
- Time-based CPT codes
- Frequent policy updates for telehealth
- Strict documentation requirements
- Variability in insurance reimbursement rules
- Pre-authorization complexities
Mental health professionals often find themselves spending more time on administrative tasks than patient care. This is where specialized mental health billing services step in.
What Does a Mental Health Billing Services Company Do?
A professional mental health billing services company handles the entire billing lifecycle, ensuring accuracy and compliance at every stage.
Core Functions Include:
- Insurance verification and eligibility checks
- Accurate coding and claim submission
- Denial management and appeals
- Payment posting and reconciliation
- Compliance monitoring
Additionally, many providers now offer integrated mental health billing and credentialing services, helping practices get enrolled with insurers faster and maintain active participation.
Why Outsourcing Mental Health Billing Makes Sense
1. Increased Revenue Collection
Outsourcing mental health billing ensures claims are submitted correctly the first time. Experienced billing teams understand payer-specific rules, which significantly reduces claim denials.
2. Focus on Patient Care
Administrative burnout is real. By choosing outsourced billing for mental health, clinicians can dedicate more time to therapy sessions instead of paperwork.
3. Access to Expertise
Specialized companies bring deep knowledge of coding and billing for mental health services, including updates in ICD-10 and CPT codes.
4. Cost Efficiency
Hiring and training an in-house billing team can be expensive. A cheap outsource mental health billing company can often deliver better results at a lower cost.
Key Components of Effective Mental Health Billing Solutions
Accurate Coding
Proper coding is the backbone of mental health medical billing. Errors in CPT or ICD-10 codes can lead to claim rejections or compliance issues.
Insurance Verification
Before a session begins, verifying patient eligibility avoids surprises later. This step is crucial in billing for mental health therapists.
Timely Claim Submission
Delays in submission can result in missed reimbursement windows. Efficient billing services for mental health clinics ensure claims are filed promptly.
Denial Management
Even the best systems face denials. The difference lies in how quickly and effectively they are resolved.
Real-World Example: Small Practice Turnaround
A behavioral health clinic in Texas struggled with delayed reimbursements and high denial rates. Their internal team lacked expertise in billing Medicare for mental health services, leading to frequent errors.
After switching to a professional behavioral and mental health billing services provider:
- Claim acceptance rate increased by 30%
- Revenue improved within 90 days
- Administrative workload dropped significantly
This highlights the impact of choosing the best outsource mental health billing and coding services.
Challenges in Mental Health Billing
Even experienced providers face obstacles:
Changing Regulations
Mental health billing is heavily influenced by federal and state policies. Keeping up with changes is critical.
Telehealth Billing Confusion
Post-pandemic, telehealth remains widely used—but billing rules vary by payer.
Documentation Errors
Incomplete or incorrect documentation often leads to claim denials.
Credentialing Delays
Without proper credentialing services, providers may face delays in receiving payments.
The Role of Technology in Mental Health Billing
Modern mental health billing solutions are powered by advanced tools:
- AI-driven claim scrubbing
- Automated eligibility verification
- Real-time reporting dashboards
- Integrated EHR systems
These tools improve accuracy and provide actionable insights into financial performance.
Integrating Medical Billing and Coding Services
To achieve optimal results, mental health practices must align their billing processes with professional medical billing services and medical coding services.
Why Integration Matters:
- Reduces coding errors
- Improves claim acceptance rates
- Enhances compliance
- Streamlines workflow
Combining medical billing and coding services ensures a seamless process from patient intake to final payment.
Revenue Cycle Management: The Bigger Picture
Mental health billing is just one part of a larger system—revenue cycle management services.
Key Stages of Revenue Cycle:
- Patient registration
- Insurance verification
- Charge capture
- Claim submission
- Payment posting
- Denial management
Efficient revenue cycle management services help practices maintain financial stability and predictability.
Credentialing: The Foundation of Successful Billing
Credentialing services play a vital role in ensuring providers can bill insurance companies legally and efficiently.
Without proper credentialing:
- Claims may be rejected
- Payments may be delayed
- Compliance risks increase
A comprehensive approach that includes mental health billing and credentialing services ensures smoother operations from the start.
Choosing the Right Mental Health Billing Partner
Not all billing companies are created equal. Here’s what to look for:
Industry Experience
Choose a provider specializing in mental health billing, not general billing.
Transparency
Clear reporting and communication are essential.
Compliance Expertise
Ensure the company stays updated with HIPAA and payer regulations.
Scalability
Your billing partner should grow with your practice.
Signs You Need to Outsource Your Billing
- Frequent claim denials
- Delayed reimbursements
- Overworked staff
- Revenue inconsistencies
- Difficulty handling billing Medicare for mental health services
If these sound familiar, it may be time to consider outsourcing mental health billing.
Future Trends in Mental Health Billing
The future of billing services for mental health is evolving rapidly:
- Increased use of automation
- Expansion of telehealth billing
- Value-based care models
- Greater emphasis on compliance
Practices that adapt early will gain a competitive edge.
A Practical Approach to Improving Billing Efficiency
Here are some actionable steps:
- Conduct regular billing audits
- Train staff on updated coding practices
- Use integrated software systems
- Partner with experienced billing providers
These steps can significantly improve overall performance.
Bringing It All Together
A well-structured billing system is the backbone of any successful mental health practice. From accurate coding to efficient claim management, every step matters.
Partnering with a trusted provider like 247 medical billing services can help practices simplify complex workflows. By combining expertise in medical billing services, medical coding services, and medical billing and coding services, along with robust revenue cycle management services and reliable credentialing services, practices can achieve consistent growth without administrative stress.
Conclusion
In today’s fast-paced healthcare environment, mental health providers cannot afford inefficient billing systems. A professional mental health billing services company offers more than just claim submission—it provides a pathway to financial stability, compliance, and growth.
Whether you're a solo therapist or a large behavioral health clinic, investing in expert mental health billing solutions can transform your practice from struggling with paperwork to thriving with predictable revenue.
FAQs
1. What makes mental health billing different from general medical billing?
Mental health billing involves time-based codes, strict documentation, and unique payer rules, making it more complex than general medical billing.
2. Is outsourcing mental health billing cost-effective?
Yes, outsourcing often reduces overhead costs while improving claim accuracy and revenue collection.
3. How do mental health billing services reduce claim denials?
They use experienced coders, advanced tools, and payer-specific knowledge to ensure accurate claim submission.
4. What are mental health billing and credentialing services?
These services include enrolling providers with insurance companies and managing billing processes to ensure smooth reimbursements.
5. Can small practices benefit from outsourced billing?
Absolutely. Even solo practitioners can improve efficiency and revenue by outsourcing billing for mental health services.
6. How long does it take to see results after outsourcing billing?
Most practices notice improvements in claim acceptance and revenue within 60–90 days.
- Art
- Causes
- Crafts
- Dance
- Drinks
- Film
- Fitness
- Food
- الألعاب
- Gardening
- Health
- الرئيسية
- Literature
- Music
- Networking
- أخرى
- Party
- Religion
- Shopping
- Sports
- Theater
- Wellness



