Why Choosing the Best Mental Health Billing Company in New York Matters More Than Ever
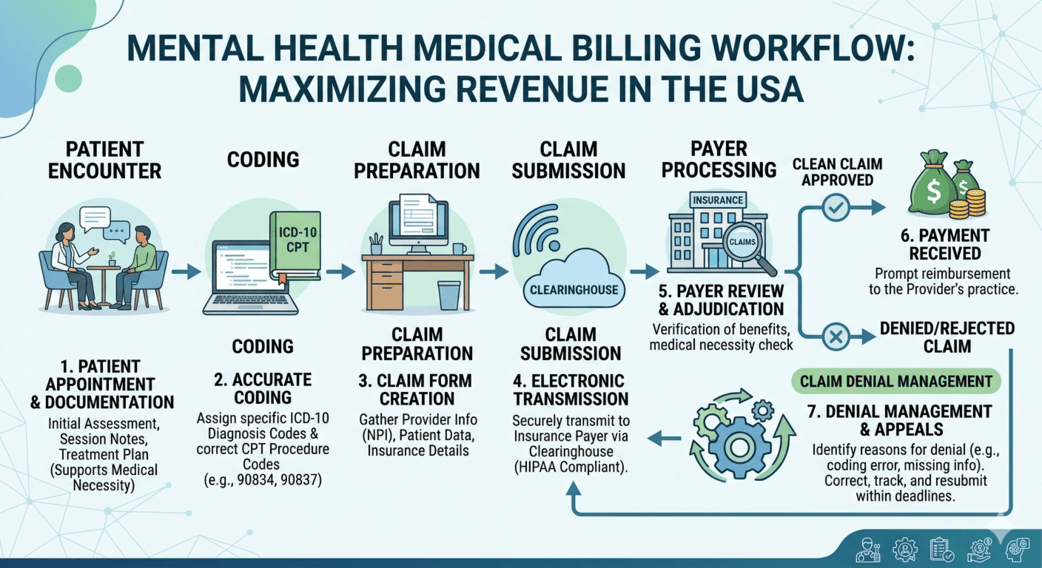
Mental health practices across New York are under pressure from every direction. Reimbursement rules keep changing, payer requirements are becoming stricter, and therapists are spending more time fixing claim issues than focusing on patient care. What once felt manageable with a small in-house team now often turns into delayed payments, denied claims, and administrative burnout.
For many behavioral health providers, billing is no longer just a back-office task. It directly affects patient retention, staff stability, cash flow, and long-term growth.
That is why more clinics, solo therapists, psychiatrists, psychologists, and counseling centers are searching for the best mental health billing company New York has to offer. The right billing partner does more than submit claims. It helps practices reduce denials, improve reimbursement accuracy, stay compliant, and create a smoother experience for both providers and patients.
The mental health industry operates differently from many other medical specialties. Session-based care, recurring appointments, authorization requirements, telehealth billing, and evolving payer policies all require specialized knowledge. A general billing vendor may understand healthcare billing overall, but behavioral health requires a far more detailed and nuanced approach.
The Billing Challenges Unique to Mental Health Practices
Mental health billing is rarely straightforward. Providers often deal with issues that do not affect other specialties at the same scale.
Consider a therapist managing multiple weekly sessions for dozens of patients. One missed authorization update or incorrect CPT modifier can delay reimbursement for weeks. If this happens repeatedly, revenue loss becomes significant.
New York practices also face additional complexities because of:
- Commercial insurance variations
- Medicaid regulations
- Telepsychiatry billing changes
- Credentialing delays
- Documentation compliance requirements
- Frequent policy updates for behavioral health coverage
A practice may deliver excellent patient care and still struggle financially because claims are not processed correctly.
This is where professional mental health insurance billing services become essential rather than optional.
What Separates a Specialized Mental Health Billing Partner From a General Billing Company?
Not every billing company understands behavioral healthcare. The difference becomes obvious when denial rates start climbing.
A specialized mental health billing specialist understands:
Session-Based Coding Complexity
Mental health coding depends heavily on session duration, treatment type, documentation quality, and payer guidelines. Codes for psychotherapy, medication management, family therapy, group sessions, and telehealth services each have unique billing requirements.
Incorrect code combinations can trigger denials immediately.
Authorization Management
Many behavioral health services require ongoing authorization tracking. Missing even a single renewal deadline can interrupt reimbursement cycles.
Experienced mental health medical billing services providers actively monitor these timelines rather than waiting for denials to occur.
Behavioral Health Documentation Standards
Insurance companies increasingly audit therapy documentation. Notes must support medical necessity while remaining compliant with payer standards.
A knowledgeable mental health billing and coding company helps ensure documentation aligns with reimbursement requirements without disrupting clinical workflows.
Why More New York Providers Are Outsourcing Billing
Several years ago, many small practices attempted to manage billing internally. Today, that model is becoming harder to sustain.
Hiring and retaining experienced billing staff is expensive. Training takes time. Turnover creates disruptions. Software upgrades add ongoing costs.
As a result, many practices now outsource mental health billing services to specialized teams that already understand behavioral health reimbursement systems.
The advantages are practical and measurable.
Faster Claims Processing
Professional billing teams typically use streamlined workflows, automation tools, and payer-specific protocols that reduce submission delays.
When claims go out correctly the first time, reimbursements arrive faster.
Lower Denial Rates
One New York counseling group struggled with a denial rate close to 18%. After transitioning to outsourced mental health billing, the practice identified recurring issues tied to authorization tracking and coding inconsistencies.
Within several months, denials dropped significantly, improving monthly cash flow without increasing patient volume.
Reduced Administrative Burden
Therapists should not spend evenings chasing insurance companies or correcting rejected claims. Outsourcing allows providers to focus more on patient care rather than administrative troubleshooting.
Improved Revenue Visibility
Many practices operate without a clear understanding of their true financial performance. A quality mental health medical billing solution provides reporting dashboards, aging analysis, denial tracking, and reimbursement insights that help practice owners make informed decisions.
Signs Your Current Billing Process Is Hurting Your Practice
Some billing problems develop slowly, making them easy to overlook.
Here are common warning signs that a practice may need a better billing partner:
Payments Are Frequently Delayed
Consistent delays often indicate workflow inefficiencies, incomplete claims, or payer follow-up issues.
Staff Spend Too Much Time on Insurance Calls
When front-office employees spend hours resolving claim problems, patient scheduling and service quality can suffer.
Denials Keep Repeating for Similar Reasons
Recurring denial patterns usually point to systemic billing issues rather than isolated mistakes.
Revenue Feels Unpredictable
Unstable cash flow often reflects inconsistent billing operations or weak accounts receivable management.
Providers Feel Burned Out
Administrative overload is a major contributor to provider stress in behavioral healthcare settings.
A strong mental health billing services agency helps stabilize operations so clinicians can focus on care delivery instead of insurance administration.
What the Best Mental Health Billing Company in New York Typically Offers
The most effective billing partners do far more than basic claim submission.
Insurance Verification Before Appointments
Eligibility issues are among the most preventable billing problems. Verifying benefits before sessions helps reduce claim rejections and unexpected patient balances.
Accurate Coding Support
Behavioral health coding changes regularly. Strong billing teams stay updated on payer rules, CPT revisions, and telehealth regulations.
Denial Management and Appeals
Denied claims should never sit untouched for weeks. The best mental health billing agency actively investigates denials, files appeals, and tracks resolution progress.
Credentialing Assistance
Many providers underestimate how much revenue is lost during credentialing delays.
Efficient credentialing processes help providers become in-network faster and avoid reimbursement interruptions.
Patient Billing Transparency
Confusing patient statements can damage trust. A professional billing company helps practices maintain clear communication regarding balances, copays, and payment expectations.
The Growing Importance of Telehealth Billing Expertise
Teletherapy and telepsychiatry changed behavioral healthcare permanently. While virtual care expanded access, it also introduced billing complexities.
Different payers apply different rules regarding:
- Telehealth modifiers
- Place-of-service requirements
- Audio-only coverage
- Cross-state licensing rules
- Documentation standards
A billing team unfamiliar with these nuances can unintentionally create reimbursement problems.
Many providers now prioritize finding a top outsource mental health billing company that specifically understands virtual behavioral healthcare billing.
Small Practices vs. Large Behavioral Health Groups
Billing challenges vary depending on practice size.
Solo Therapists
Independent therapists often need simplified workflows, affordable support, and help managing insurance complexity without hiring full administrative teams.
Billing services for mental health therapists can help solo providers maintain profitability while minimizing administrative strain.
Multi-Provider Clinics
Larger practices usually need:
- Advanced reporting
- Multi-location billing coordination
- Authorization management
- Staff performance tracking
- Revenue cycle optimization
The right mental health medical billing services outsourcing partner adapts based on practice scale rather than offering rigid one-size-fits-all systems.
Questions to Ask Before Hiring a Billing Company
Not all billing vendors deliver the same level of expertise. Before choosing a partner, behavioral health providers should ask detailed operational questions.
Do They Specialize in Mental Health?
General healthcare billing experience is not enough. Behavioral health requires dedicated expertise.
How Do They Handle Denials?
A company that only submits claims without proactive denial management may create long-term revenue problems.
What Reporting Is Available?
Providers should have visibility into collections, aging reports, denial trends, and reimbursement performance.
Who Handles Insurance Follow-Ups?
Some companies outsource follow-up work overseas, which can create communication delays and payer inefficiencies.
Can They Support Growth?
As practices expand, billing systems must scale accordingly.
The best mental health billing company New York providers choose is often one that acts as a long-term operational partner rather than simply a vendor.
The Financial Impact of Better Billing Operations
Efficient billing directly affects practice sustainability.
A practice collecting even 8–10% more revenue due to cleaner claims and stronger denial management can significantly improve profitability over time.
That additional revenue may help fund:
- Additional therapists
- Better patient support systems
- Expanded telehealth services
- Improved staff retention
- Technology upgrades
In behavioral healthcare, operational efficiency often determines whether a practice can grow responsibly without sacrificing care quality.
Compliance Cannot Be Overlooked
Behavioral health records contain highly sensitive patient information. Billing processes must comply with strict privacy and security standards.
Professional mental health insurance billing services providers typically maintain secure systems, HIPAA-compliant workflows, encrypted communication protocols, and ongoing compliance monitoring.
Practices should never assume compliance happens automatically. Billing errors tied to privacy or documentation issues can create serious financial and legal risks.
Why Relationship Quality Matters
Technology matters, but communication matters just as much.
Many providers become frustrated when billing companies feel unreachable or unresponsive. Delayed answers create anxiety, especially when revenue concerns arise.
A reliable billing partner should provide:
- Dedicated account management
- Transparent communication
- Regular performance reviews
- Quick issue resolution
- Collaborative problem-solving
Strong partnerships often feel like an extension of the practice itself.
FAQs
What does a mental health billing company actually do?
A mental health billing company manages insurance verification, coding, claim submission, payment posting, denial management, appeals, reporting, and reimbursement tracking for behavioral health providers.
Why is behavioral health billing more complicated than general medical billing?
Behavioral health billing involves recurring therapy sessions, authorization requirements, evolving telehealth rules, time-based coding, and strict documentation standards that vary across payers.
Is outsourced mental health billing cost-effective for small practices?
In many cases, yes. Outsourced mental health billing can reduce staffing costs, improve claim accuracy, minimize denials, and free providers from administrative burdens.
How can providers reduce claim denials?
Reducing denials usually requires accurate coding, eligibility verification, authorization tracking, timely claim submission, and consistent payer follow-up.
What should therapists look for in a billing partner?
Therapists should prioritize behavioral health expertise, transparent reporting, communication quality, denial management processes, compliance standards, and scalability.
Can a billing company help with credentialing?
Many specialized providers also offer credentialing services to help therapists and psychiatrists become in-network with insurance carriers more efficiently.
Final Thoughts
Behavioral healthcare providers face growing operational demands, and billing complexity continues to increase each year. Practices that rely on outdated systems or generalized billing support often experience unnecessary financial pressure, staff burnout, and inconsistent reimbursements.
Choosing the right partner is not simply about outsourcing paperwork. It is about creating stability, improving revenue performance, and protecting the long-term health of the practice itself. Whether a provider operates independently or manages a large behavioral health organization, specialized support can make a meaningful difference.
Companies like 247 Medical Billing Services have become part of this evolving landscape by helping behavioral health providers navigate medical billing services, medical coding services, medical billing and coding services, revenue cycle management, and credentialing services with greater efficiency and accuracy. For practices seeking a more dependable operational foundation, working with an experienced behavioral health billing partner can support both financial performance and better patient care outcomes.
- Art
- Causes
- Crafts
- Dance
- Drinks
- Film
- Fitness
- Food
- Juegos
- Gardening
- Health
- Home
- Literature
- Music
- Networking
- Other
- Party
- Religion
- Shopping
- Sports
- Theater
- Wellness



