The Complete Guide to Mental Health Insurance Billing in the USA: Challenges, Solutions, and Growth Strategies
Introduction
Mental health practices across the USA are experiencing a steady rise in demand, but behind every successful therapy session lies a complex administrative process—mental health insurance billing. From verifying benefits to submitting accurate claims and handling denials, billing can quickly become overwhelming for therapists and clinics.
Unlike other medical specialties, mental health billing involves unique coding structures, evolving payer rules, and strict compliance requirements. When done incorrectly, it can lead to delayed payments, claim denials, and revenue loss.
This guide breaks down everything providers need to know about mental health insurance billing, while also exploring how modern solutions and outsourcing can streamline operations and improve financial performance.
Understanding Mental Health Insurance Billing
At its core, mental health insurance billing is the process of submitting claims to insurance companies for services like psychotherapy, psychiatric evaluations, and counseling sessions.
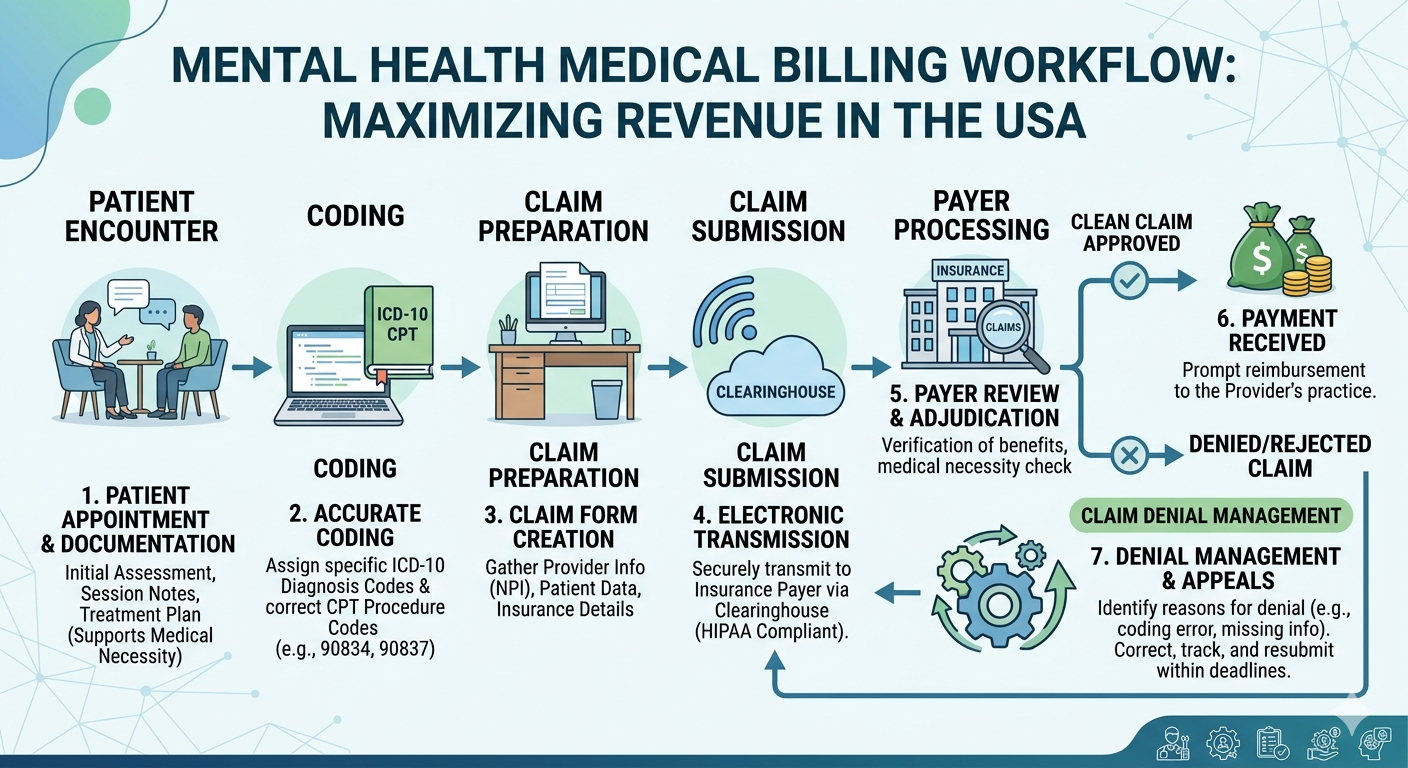
However, it’s not as simple as sending an invoice. The process involves:
- Patient eligibility verification
- Accurate CPT and ICD-10 coding
- Claim submission and tracking
- Payment posting
- Denial management and appeals
A mental health billing specialist plays a crucial role in ensuring each of these steps is handled correctly to maximize reimbursements.
Why Mental Health Billing Is More Complex Than General Medical Billing
Mental health billing differs from other specialties due to several factors:
1. Frequent Coding Updates
Therapy services use time-based CPT codes, which require precise documentation. Even a small error can lead to claim rejection.
2. Insurance Limitations
Many insurance plans in the USA have:
- Session limits
- Pre-authorization requirements
- Coverage restrictions for certain therapies
3. Confidentiality Regulations
Mental health records are highly sensitive, requiring strict adherence to HIPAA compliance.
4. High Denial Rates
Incorrect coding, missing documentation, or authorization issues can increase denials.
Because of these complexities, many providers turn to mental health medical billing services to handle the workload efficiently.
Key Components of an Effective Billing Process
A well-structured billing system ensures consistent cash flow and fewer disruptions. Here’s what an optimized process looks like:
Eligibility Verification
Before the appointment, confirming insurance coverage prevents surprises later.
Accurate Coding
Using proper CPT and ICD-10 codes ensures claims are accepted. This is where medical coding services become essential.
Timely Claim Submission
Submitting claims quickly reduces delays in reimbursement.
Payment Posting
Tracking payments ensures accuracy in accounts receivable.
Denial Management
Identifying and correcting denied claims improves revenue recovery.
When combined, these steps form a solid revenue cycle management services framework.
The Role of Mental Health Billing Specialists
A mental health billing specialist is not just a biller—they’re a financial gatekeeper for your practice.
Their responsibilities include:
- Managing insurance claims end-to-end
- Staying updated with payer policies
- Handling appeals and re-submissions
- Ensuring compliance with federal and state regulations
In many cases, practices rely on mental health billing companies to access experienced specialists without hiring in-house staff.
Benefits of Outsourcing Mental Health Billing Services
Many providers in the USA are now choosing to outsource mental health billing services instead of managing billing internally.
1. Reduced Administrative Burden
Therapists can focus on patient care instead of paperwork.
2. Improved Revenue Collection
Experienced teams minimize errors and speed up reimbursements.
3. Cost Efficiency
Outsourcing eliminates the need for hiring, training, and maintaining in-house billing staff.
4. Access to Expertise
A mental health billing services agency stays updated with industry changes and payer requirements.
5. Scalability
As your practice grows, outsourced teams can scale with your needs.
This is why many providers search for the best mental health billing agency or a top outsource mental health billing company to support their operations.
What to Look for in a Mental Health Billing Agency
Choosing the right partner is critical. Not all mental health billing agencies offer the same level of service.
Here are key factors to consider:
Industry Experience
Look for agencies specializing in billing services for mental health providers.
Compliance Knowledge
Ensure they follow HIPAA and payer-specific guidelines.
Transparent Reporting
Regular financial reports help track performance.
Technology Integration
Modern billing systems improve accuracy and efficiency.
End-to-End Services
The best agencies offer complete mental health medical billing solution, including coding, billing, and RCM.
Real-World Example: Small Practice Growth Through Outsourcing
A small therapy clinic in Texas struggled with delayed payments and frequent claim denials. Their in-house billing system lacked expertise in mental health coding.
After switching to outsourced mental health billing, they experienced:
- 30% reduction in claim denials
- Faster reimbursement cycles
- Improved patient satisfaction due to smoother billing
This shift allowed therapists to focus entirely on patient care while the billing agency handled financial operations.
The Importance of Medical Billing and Coding Integration
Successful billing depends heavily on the accuracy of coding.
Combining medical billing and coding services ensures:
- Correct procedure codes
- Proper diagnosis linkage
- Reduced claim rejections
A well-integrated system connects coding directly with billing workflows, improving overall efficiency.
How Revenue Cycle Management Strengthens Mental Health Practices
A complete revenue cycle management services approach goes beyond billing.
It includes:
- Patient scheduling optimization
- Insurance verification
- Charge capture
- Claims processing
- Payment collection
For mental health providers, RCM ensures financial stability and predictable revenue streams.
Credentialing: The Foundation of Insurance Billing
Before billing even begins, providers must be enrolled with insurance companies. This is where credentialing services come into play.
Credentialing ensures:
- Providers are authorized to bill insurers
- Faster claim approvals
- Reduced risk of payment delays
Without proper credentialing, even correctly submitted claims may be denied.
Common Challenges in Mental Health Insurance Billing
Even experienced providers face obstacles:
- Frequent policy changes by insurers
- Complex authorization requirements
- High claim denial rates
- Administrative overload
Working with a mental health billing and coding company helps overcome these challenges through expertise and streamlined processes.
Future Trends in Mental Health Billing
The industry is evolving rapidly, with trends such as:
Telehealth Billing Expansion
More insurers now cover virtual therapy sessions.
Automation and AI Tools
Billing software is improving accuracy and reducing manual work.
Value-Based Care Models
Reimbursement is increasingly tied to patient outcomes.
Increased Demand for Outsourcing
More practices are adopting mental health medical billing services outsourcing for efficiency.
Choosing the Right Billing Partner for Long-Term Success
Selecting a reliable partner is not just about cost—it’s about long-term growth.
A strong mental health billing agency should:
- Align with your practice goals
- Offer customized solutions
- Provide ongoing support
- Ensure compliance and transparency
Conclusion
Navigating mental health insurance billing in the USA requires precision, expertise, and adaptability. From handling complex coding requirements to managing insurance claims and ensuring compliance, the process can be overwhelming without the right support.
This is where experienced providers like 247 medical billing services play a valuable role. By offering comprehensive medical billing services, medical coding services, and integrated medical billing and coding services, they help streamline operations for mental health practices. Their expertise in revenue cycle management services ensures consistent cash flow, while reliable credentialing services lay the groundwork for smooth insurance processing.
For mental health providers looking to grow sustainably, partnering with the right billing experts can make all the difference—transforming administrative challenges into opportunities for efficiency and success.
FAQs
1. What is mental health insurance billing?
Mental health insurance billing is the process of submitting claims to insurance companies for therapy and psychiatric services, ensuring providers receive payment for their services.
2. Why should I outsource mental health billing services?
Outsourcing reduces administrative workload, improves claim accuracy, and increases revenue by minimizing denials and delays.
3. What does a mental health billing specialist do?
They manage the entire billing process, including coding, claim submission, payment tracking, and denial resolution.
4. How do mental health billing companies improve revenue?
They use expertise and advanced systems to reduce errors, speed up reimbursements, and optimize the billing process.
5. What are the benefits of revenue cycle management services?
RCM services streamline the entire financial process, from patient intake to final payment, ensuring consistent cash flow.
6. How important are credentialing services in billing?
Credentialing is essential because it allows providers to bill insurance companies and receive payments without delays or rejections.
- Art
- Causes
- Crafts
- Dance
- Drinks
- Film
- Fitness
- Food
- Games
- Gardening
- Health
- Home
- Literature
- Music
- Networking
- Other
- Party
- Religion
- Shopping
- Sports
- Theater
- Wellness



